
Your Pregnancy Journey From Planning to Parenthood
– A Gentle Guide
Pregnancy is one of life’s most beautiful journeys. Starting before conception and continuing well after birth, every stage brings new changes and joys. This guide walks you through what to expect, how to care for yourself and your baby, and when to reach out for support.
Pre-Pregnancy Building the Best Foundation
(3–6 Months Before Trying)
The healthiest pregnancies often begin months before a positive test. Giving your body time to prepare reduces risks and helps everything start smoothly.
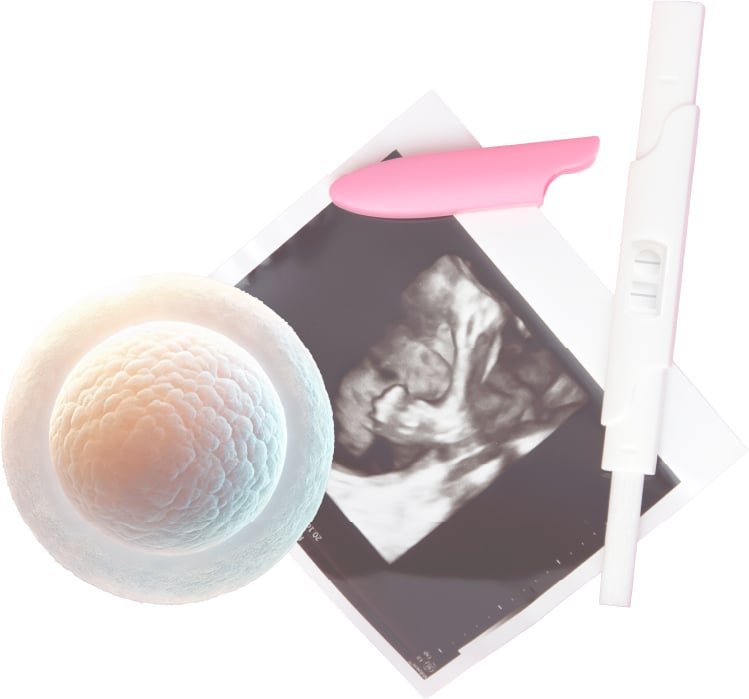
Pre-pregnancy counselling
with your doctor
Key Steps Include:
Optimising any existing
conditions
(e.g., diabetes, thyroid, high blood pressure)
Dental check-up
(gum health matters more than you think)
STI screening or genetic carrier testing if relevant
Lifestyle changes that make a big difference
Stop smoking, alcohol, and recreational drugs completely
Limit caffeine to 200 mg/day (about 1–2 cups of coffee)
Eat nutrient-rich meals with plenty of fruits, vegetables, whole grains, and protein
Exercise regularly (aim for 150 minutes
of moderate activity per week)
Track ovulation if you want to
conceive soon
Supplements &
Protection
Start folic acid (400 mcg daily, higher dose if having risk factors) at least 3 months before
Check immunity for rubella, chickenpox, COVID-19, and flu – update vaccines as needed
Discuss any current medications
with your doctor (some like retinoids, certain blood pressure drugs, or anti-seizure medicines need safe alternatives)


If you have irregular periods, severe pelvic pain, or known fertility concerns,
come in early – we can help sooner
First Trimester
The Quiet, Crucial Beginning
These early weeks are full of rapid changes – and early care makes all the difference.


Confirm the pregnancy is in the right place (rule out ectopic)
What Happends
Accurate dating scan
Antenatal blood tests, NIPT (if chosen), First trimester screening - includes - pre-eclampsia screening, Nuchal translucency (NT) scan.
* Continue folic acid until week 12, then review whether to add low-dose aspirin and vitamin D if indicated.
Check fetal heart activity (usually visible by 6–7 weeks)
By Weeks:
First antenatal visit, routine exam, start folic acid
5-10 weeks


11-14 weeks




0-14
weeks
Second Trimester
Feeling the Glow
Often called the “honeymoon phase” – energy returns, nausea fades, and you start to feel baby move.
Key ultrasounds & checks:
Gender (if visible and desired)
16 weeks






15-28
weeks


18-22 weeks
Detailed anomaly scan checks baby’s organs and development)
24-28 weeks
Growth scan, amniotic fluid check, placenta position






Important Actions
Oral glucose tolerance test
(screen for gestational diabetes)
Dental check-up
Influenza vaccine
Tdap vaccine (protects baby from whooping cough)
Haemoglobin check
Nutrition Boost
Add DHA (for brain development)
Iron tablets
Calcium from week 20 (if needed)
Extra ~340 calories/day
Third Trimester
Getting Ready for Birth
Baby is growing fast, and your body is preparing for labour.
Growth, fluid, placenta check (± 3D/4D)
28-32 weeks






29-40+
weeks
32-37 weeks
Growth, estimated fetal weight, Doppler if needed




To-Dos
Haemoglobin check
Tdap vaccines (27weeks)
RSV vaccines (32 weeks)
Group B Streptococcus (GBS) screening - if needed
Perineal massage (from 34 weeks – helps reduce tearing)
Discuss birth plan, pain relief options, and delivery timing
Nutrition & Comfort
Continue DHA, iron, calcium, vitamin D
Extra ~450 calories/day
Gentle movement, hydration, rest
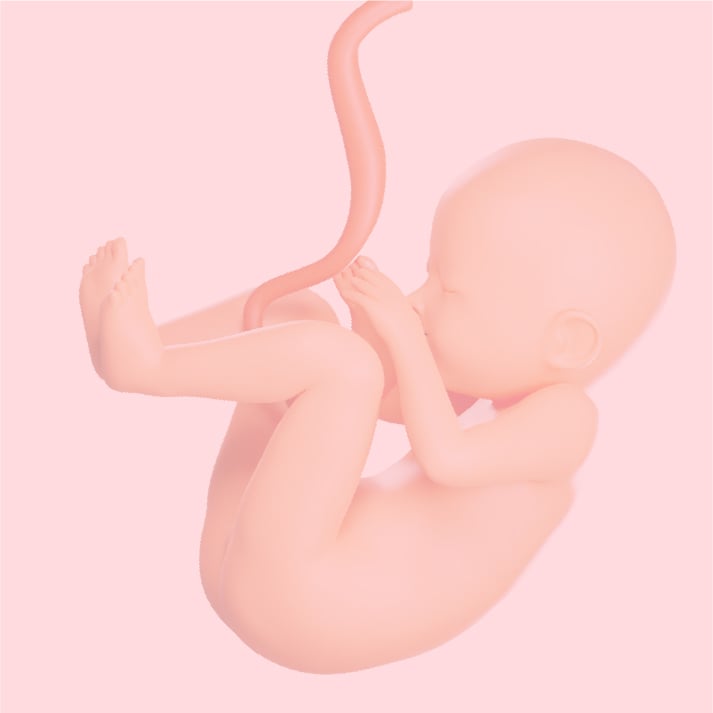
Delivery Day
What to Expect
Delivery is when you finally meet your baby. Most births happen vaginally (normal delivery), but a Caesarean section (C-section) may be needed or planned for safety. Your care team will guide you every step
Vaginal Delivery
(Normal Delivery)
Vaginal delivery is the birth of a baby through the vagina following labor, with the uterus contracting to help deliver the baby.
Instrumental Delivery
Sometimes assistance is needed using vacuum extraction or forceps, usually during the second stage if progress is slow or there are fetal concerns.
[NOTE] In some cases, it may be necessary to convert to an emergency C-section (EMLSCS)
First Stage – Labor:
Latent phase:
Early contractions cause gradual cervical thinning and opening up to ~4–6 cm. This phase can last many hours.
Active phase:
Stronger, frequent contractions (about 4 in 10 minutes) open the cervix from ~4–6 cm to 10 cm, typically at a rate of ~1 cm per hour.
Second Stage
Pushing and Birth: You actively push to move the baby through the birth canal. This usually lasts from a few minutes to a few hours.
Third Stage
Placenta Delivery: The placenta is expelled, usually within 5–30 minutes after birth.
Caesarean Delivery
(C-Section)
The baby is delivered through an incision in your abdomen and uterus. It can be planned (elective) or done in an emergency.
Experience: You are awake (using spinal/epidural anesthetic) and feel pressure, but no pain
Duration: The procedure typically takes 40–60 minutes.
Pain Relief Choices
You have options to manage
comfort throughout the process:
Natural Methods:
Breathing techniques,
movement, and massage.
Medical Options:
Gas (Entonox), injections,
or an epidural.
When Should You Go to the Hospital?
Go to the hospital if you have:
• Regular, painful contractions
• Leaking liquor (water breaking)
• Bloody show
• Reduced or no fetal movement
When in doubt, check it out.
Postnatal Recovery
Caring for Yourself After Birth
The first weeks are for healing, bonding, and adjusting.


Postnatal check-ups focus on
• Wound healing (if caesarean or episiotomy)
• Physical & emotional well-being
• Breastfeeding support
• Contraception options
• Pelvic floor exercises
When to seek urgent help
Heavy bleeding
or large clots
Foul-smelling
discharge
Fever
Severe breast
pain/redness
Leg pain/swelling
Persistent low
mood or anxiety
Plan ahead aim for at least a
2-year gap before the next pregnancy for full recovery.
Disclaimer: The information provided in this website represents the views and opinions of the original creator. The information provided is intended for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. It's important to note that this website does not advocate for or endorse any specific tests, products, procedures, opinions, or information mentioned within its content. Always seek the advice of your physician or another qualified health provider for any questions you may have regarding a medical condition.
2026 All rights reserved © Dr Ng Ying Shan
免责声明:此网站提供的信息仅代表原始创作者的观点和意见。此网站提供的信息仅供参考,不旨在替代专业医学建议、诊断或治疗。此网站不主张或支持其内容中提及的任何特定测试、产品、程序、观点或信息。当您遇到任何健康问题时,请咨询您的医生或其他合格的医疗专业人员,,进行诊断与治疗。
